

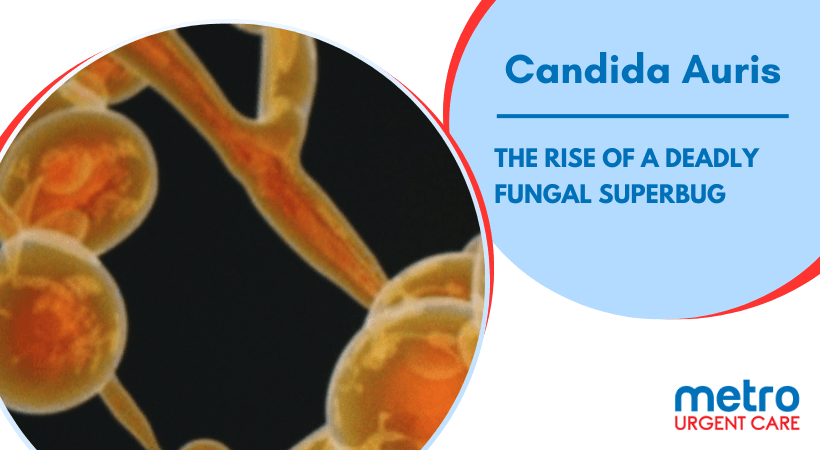
Candida Auris, a relatively unknown fungal infection recently discovered a decade ago, has emerged as a formidable superbug, causing deadly infections treated in hospitals and healthcare facilities worldwide. This multidrug-resistant fungus can survive on surfaces for weeks, making it extremely difficult to contain. According to recent studies, the global contraction of C. Auris infections has increased exponentially, with mortality rates ranging from 30% to 60%. In addition, studies have shown that this fungus can transfer its drug-resistant genes to other Candida species, increasing the risk of further outbreaks.
The emergence of Candida Auris has posed a significant challenge to global public health and requires urgent attention to prevent further spread. Here is everything to learn about this deadly fungal infection to inform you of how to take an effective Candida auris treatment to cast your concerns aside!
Candida Auris, often called C. Auris, is a tiny fungus belonging to the family Candida. In short, candida is a yeast infection. Microorganisms called Candida can occur in a broad spectrum of species. Many dwell on your skin or within your body - though these are harmless.
C. Auris was first identified in 2009 and has since spread rapidly across the globe, causing severe infections in hospitalized patients and those with weakened immune systems. It survives on surfaces for weeks, contributing to its spread in healthcare facilities. Due to its emergence as a global health threat, C. Auris requires increased attention and effective control measures.
Candida Auris can be spread by various means, including direct contact with infected people or contaminated surfaces, including through the air. It has been discovered that the fungus can survive on hospital premises for weeks, which helps to facilitate its spread throughout healthcare institutions. Infested medical devices like ventilators and catheters can also transfer the disease. Furthermore, research has demonstrated that C. Auris can spread from one patient to another, particularly when infection prevention and control measures are insufficient. C. Auris is a serious public health risk due to its ease of dissemination and resistance to most antifungal medications. Effective infection control techniques are required to prevent its spread.
Candida Auris can live on surfaces for longer periods than other funguses or contaminates, extending to several weeks in certain instances. This lifespan aids in its spread within healthcare institutions where the fungus can contaminate surfaces and equipment, exponentially making it easier to spread.
Candida Auris symptoms can vary depending on the severity and location of the infection. Some people may not experience symptoms, while others may develop serious and potentially life-threatening complications. Here are some common symptoms associated with Candida Auris infection:
These symptoms are nonspecific and can be caused by other infections or medical conditions. Therefore, laboratory testing is necessary to confirm a Candida Auris infection. Early diagnosis and treatment are crucial to prevent the spread of the infection, better improving the outcomes for affected individuals.
Candida Auris is a yeast that may trigger infections in humans. Although the precise etiology of Candida Auris infection is unknown, it is thought to be transmitted from person to person or by contaminated equipment and surfaces in medical facilities.
People with impaired immune systems, those who have recently undergone surgery or been hospitalized, and those who have taken antibiotics or antifungal drugs are more likely to contract this infection.
Most C. auris occur in persons with several chronic or recurring illnesses. The risk of C. Auris infection is significantly higher in those who reside in nursing homes or frequently visit hospitals.
Additional risks consist of the following:
Here are the commonly used means to diagnose C. Auris:
Despite the severity of C. Auris infections, most of them are curable. Usually, echinocandins, an antifungal medication, are used as the first line of treatment. Treatment-resistant strains may cause more serious infections and may challenge the treatment. In these circumstances, doctors prescribe various antifungal medications at high doses to eradicate the infection.
Call us or visit our walk-in clinic in Chicago, IL, and let our medical providers help you today!